ESCMID experts recently released comprehensive guidelines for the control of MDR-GNR. Working with a limited evidence base, the experts managed to compile a coherent set of guidelines with graded recommendations. Given the important differences in the epidemiology of the various species and resistance patterns of MDR-GNR, this is really a 6-for-the-price-of-one set of guidelines, with separate recommendations for: ESBL-producing Enterobacteriaceae, MDR K. pneumoniae, MDR A. baumannnii, MDR P. aeruginosa, Burkholderia cepacia and Stenotrophmonas maltophilia.
Five key interventions are identified: hand hygiene measures, active screening cultures, contact precautions, environmental cleaning, and antimicrobial stewardship. ‘Selective’ decontamination using antibiotics, topical ‘source control’ using chlorhexidine, and infrastructure / education are also reviewed. Which of these is most important? Most studies included multiple interventions simultaneously, so it’s difficult to tell and it will probably depend on species and setting.
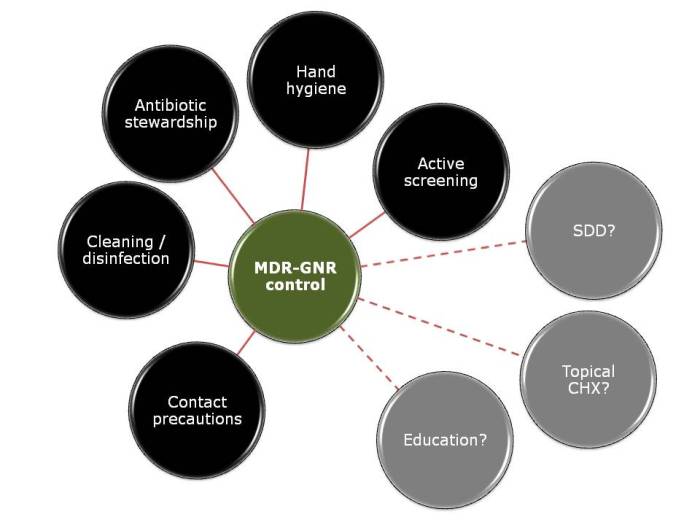 Figure: The cornerstones of MDR-GNR control (but we don’t have enough data to say which is most important, and which are redundant).
Figure: The cornerstones of MDR-GNR control (but we don’t have enough data to say which is most important, and which are redundant).
A few points for discussion:
- We still don’t really know what works to control MDR-GNR. Reflecting on my recent blog on influenza transmission, where the relative importance of various transmission routes varies by context, this also seems likely for MDR-GNR. The relative importance of say, environment vs. hands, is likely to vary by setting for a given MDR-GNR species. This makes definitive guidelines difficult to write!
- The guidelines begin with a useful review of the differing transmission routes for the various MDR-GNR species. This shows that person-to-person spread of Klebsiella species and some other Enterobacteriaceae (such as Enterobacter species and Serratia species) seems to be more important than for E. coli. The non-fermenters A. baumannii and P. aeruginosa have some fundamental differences with one another and with the Enterobacteriace in terms of transmission routes. If I had to rate the importance of patient-to-patient spread vs. other routes for the various MDR-GNR I would say A. baumannii > Klebsiella species > other Enterobacteriaceae > P. aeruginosa > E. coli. But don’t hold me to it!
- It seems odd that all of the recommendations are ‘strong’ but the evidence is graded mainly as ‘moderate’, ‘low’ or ‘very low’. Perhaps more ‘conditional’ recommendations would be a better fit with the quality of the evidence?
- The recommendations are stratified by organism-group and setting (endemic or outbreak), which is a workable approach. What you’d do in an outbreak does probably differ from what you’d do in an endemic setting.
- There’s a useful recommendation for the identification of a new CRE case to prompt contact tracing and enhanced local surveillance, in line with PHE and CDC recommendations.
- There’s a little fence sitting when it comes to a recommendation for active surveillance cultures in the endemic setting: ‘the implementation of ASC [active surveillance cultures] should be suggested only as an additional measure and not included in the basic measures to control the spread of MDR-GNB in the endemic setting.’ Still not clear whether this is a recommendation for or against ASC in the endemic setting!
- I was surprised not to see a recommendation to use a disinfectant to help bring A. baumannii outbreaks under control. I appreciate that there is little evidence in endemic settings, but controlling the environmental reservoir does seem to be important in controlling A. baumannii outbreaks.
- The remit of the guidelines is for adult patients, but what to do on neonatal units and in paediatrics?
- The guidelines are restricted to hospitalized patients, but what about long-term acute care facilities (that are riddled with CRE in some parts of the world) and long-term care facilities (that have an unknown but probably sizable burden of resistance)?
- The searches were restricted to MDR bacteria according to ECDC criteria, but what about all those literature on preventing the transmission of resistant (but not multiresistant) and sensitive GNR? If something works to control GNR, there’s no reason why it shouldn’t work to control MDR-GNR (except, perhaps, for antibiotic stewardship).
- Finally, if all else fails (and only then), consider closing the ward!
In summary, these guidelines are very well written and will provide useful guidance for those on the front line try to deal with endemic and epidemic MDR-GNR. However, above all else, they highlight the need for high-quality studies telling us what works to control MDR-GNR.