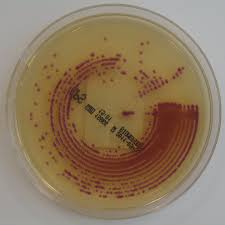
My old CIDR team have just published a study in JAC reporting a very low rate of carriage of CPE in patient admitted to a hospital in central London (just 5 (0.1%) of 4006 patients). This was a lot lower than we expected! Despite the very low rate of carriage, overseas hospitalisation was a significant risk factor for CPE carriage, and supports that we should be screening patients with recent overseas hospitalisation for CPE carriage.
CPE
CPE has landed in Manchester…officially
A really important point prevalence survey of CPE carriage in inpatients in a hospital in Manchester has just been published in the Journal of Hospital Infection. Important because of the high rate of carriage (11% of 662 patients included). Important because for every 1.6 known cases of CPE, there was an undetected case lurking, despite an extensive screening programme. Important because the lack of significant risk factors associated with CPE carriage suggests that it is distributed homogeneously, endemic in the population. And important because this is the first citable publication suggesting that Manchester has a problem with CPE, despite us having known about it for years via professional networks.
Balancing risk and resource for CPE screening
The PHE Toolkit recommends pre-emptive isolation for patients who meet one of the risk-factor triggers for CPE screening. Furthermore, the pre-emptive isolation recommended in the Toolkit should be continued until three negative screens are obtained, each separated by 48 hours. In what is best described as a data-based thought experiment, colleagues from Imperial tested the impact of various CPE screening strategies on the burden of contact precautions generated.
Colistin resistance in CPE: an emerging threat
I am becoming increasingly interested in colistin resistance in CPE, not least because of this work that we will be presenting on colistin resistance in CPE at ECCMID in a few months time. I have been brushing up on how colistin resistance occurs in CPE, and why it is important, so thought I’d share my findings. I started with a pubmed search for “colistin resistance mechanism” on 12/02/16 and this is what I found (85 hits from the initial search):
Colisin
Colistin is an old class (discovered during WWII) of cationic antibiotic. Colistin (polymyxin E) is a polypeptide bactericidal agent and is one of the two clinically available forms of polymyxin agents (polymyxin B and polymyxin E). Colistin interacts with lipopolysaccharide in the outer membrane, resulting in a leaky and ultimately dead bacterial cell.1 Issues with presumed nephrotoxicity have kept colistin very much on the top shelf, but the emergence of CPE has brought colistin down a shelf or two – and we are learning that the nephrotoxicity tradionally associated with colisin may not be so bad afterall.1
Transmissible colistin resistance – made in China
The emergence of CPE (and carbapenem-resistance in other Gram-negative bacteria) has forced us to reach to the dusty old antibiotic shelf to revive the clinical use of older agents with activity against Gram-negative bacteria, principally colistin. Colistin isn’t perfect by any means – it has poor tissue penetration compared with the carbapenems, and is associated with nephrotoxicity (although the high levels of nephrotoxicity in the older medical literature has not been reported due to better management of the drug). Furthermore, resistance has already been reported. To date – this has been mutational resistance, which does not have the capacity to spread horizontally. It was only a matter of time before a colistin resistance gene mobilised.
UK guidelines for the control of multidrug-resistant Gram-negative bacteria
The UK guidelines for the prevention and control of multidrug-resistant Gram-negative bacteria (MDR-GNB) are published this week. It’s useful that the publication of these guidelines coincides with Antibiotic Awareness Week because MDR-GNB are brining us ever closer to the end of antibiotics. Although the guidelines don’t cover the treatment of MDR-GNB (this will be addressed in a forthcoming guideline), these highly resistant MDR-GNB leave few therapeutic options. Even when they remain susceptible to some antibiotics, these antibiotics are not front-line antibiotics for a reason (including poor tissue penetration and side effects). Furthermore, we are already seeing resistance to last-line (aka end of the golden-antibiotic-road) antibiotics e.g. colistin. Therefore, the old adage that ‘prevention is better than cure’ has never been so true!
Appraising the options for detecting carbapenemase-producing organisms
Carbapenemase-producing organisms (including CPE) present important clinical challenges: the “triple threat” of high levels of antibiotic resistance, virulence, and potential for rapid spread (locally, regionally, nationally, and globally)! However, these organisms somewhat ironically also present challenges to detection in the clinical laboratory. You’d expect that since these organisms are so important clinically they’d be dead easy to detect in the clinical lab – but this isn’t the case.
A comprehensive review published in Clinical Microbiology Reviews provides an overview of the diagnostic approaches to detect carbapenemase producers in the clinical lab. Figures 6 and 7 of the review provide a useful overview of the two broad approaches you could take: culturing organisms on agar plates, or using nucleic acid amplification techniques (NAAT – most commonly PCR) directly from a rectal swab.
Guidelines to control multidrug-resistant Gram-negative bacteria: an ‘evidence-free zone’
I recently had a review published in CMI comparing EU guidelines for controlling multidrug-resistant Gram-negative bacteria (MDR-GNB). I included the following guidelines in my review: ECCMID 2014, Irish MDRO, PHE CPE, HPS CPE, ECDC systematic review on CPE (not strictly a guideline, but did include some recommendations). A couple of important points arise:
Reflections from Infection Prevention 2015 Part I: Beating the bugs
Infection Prevention 2015, the annual conference of IPS, was held in Liverpool this year. I’m delighted to say that the abstracts from the submitted science are published Open Access in the Journal of Infection Prevention. This first instalment of my report will be “bug-focussed”, followed by another two on different themes:
Part I: Beating the bugs
Part II: Improving the systems
Part III: Thinking outside the box
Opening lectures
The conference kicked off with fellow ‘Reflections’ blogger Prof Andreas Voss. By Andreas’ own admission, he was given a curve-ball of a title: ‘CRE, VRE, C. difficle or MRSA: what should be the priority of infection prevention?’ [No idea where that could have come from…] Andreas developed a framework for grading the priority of our microbial threats, accounting for transmissibility, virulence, antibiotic resistance, at-risk patients, feasibility of decolonisation, cost, and impact of uncontrolled spread. And the result? Any and all microbes that cause HCAI should be a priority of infection prevention. Even those that seem to have less clinical impact (such as VRE) are good indicators of system failure. If we focus too much on one threat, we risk losing sight of the bigger picture.
CRE -> CPE
I have thought a lot (probably too much) about the best way to describe the issue of carbapenem resistance in Enterobacteriaceae. I decided ages ago that CRE (a la the CDC) is the way to go as a generic term to describe the problem. But the more I think about it, the more I am coming around to the idea that CPE (a la PHE) is better. And here’s why:
- The real issue from a clinical and infection control viewpoint is CPE. Enterobacteriaceae that are resistant to carbapenems by means other than an acquired carbapenemase (i.e. CRE that are not carbapenemase producers) are important, but they don’t seem to have the same capacity to spread as carbapenemase producers.
- It’s a really confusing situation in terms of terminology. From the “end user” staff member on the front line and patient, all that really counts is whether it is a CPE or not. It’s really rather confusing to tell a patient that the have a “CRE that is also a carbapenemase producer” – easier just to say “you have a CPE”. (I accept that you will also need to tell a patient if they have a CRE that is not a carbapenemase producer – but I think this way around is easier.)
- CPE is already en vogue in the UK (mainly due to the PHE Toolkit) so using any other term risks confusion at the time of patient transfer. (Clearly, this point is reversed if you are working in the US!)
I still think that “CRO/CPO” is not the way to go, given the gulf in epidemiology between the Enterobacteriaceae and the non-fermenters (although, sometimes, begrudgingly, you have to go there). What I mean by this is that you will sometimes detect a carbapenemase gene from a PCR but don’t yet know whether it is from a non-fermenter or Enterobacteriaceae species. In this circumstance, this has to go down as a ‘CPO’.
So, there you have it, a personal U-turn. CRE -> CPE. But I wonder whether CDC and PHE and the international community will ever agree a common term…