This time last week, we were on red alert that a MERS-CoV pandemic was gathering pace. The news over the last few days has been more encouraging, with no new cases reported in Saudi Arabia, the epicenter of the MERS-CoV cases. However, there are still plenty of patients with MERS-CoV who need to be cared for around the world. Like SARS-CoV, but unlike the “usual suspects” that cause HCAI such as MRSA and C. difficile, MERS-CoV has the capacity to affect both healthcare workers and patients. Thus, I hope that this ‘survival guide’ will prove useful to those on the front line.
I presented a webinar on ‘MERS-CoV: coming to a hospital near you? Infection prevention and control challenges’. You can download the slides here. I came across a fantastic blog whilst preparing the webinar: ‘Virology Down Under’ by Dr Ian Mackay. I’ve used some of his excellent images in the slides, with his kind permission.
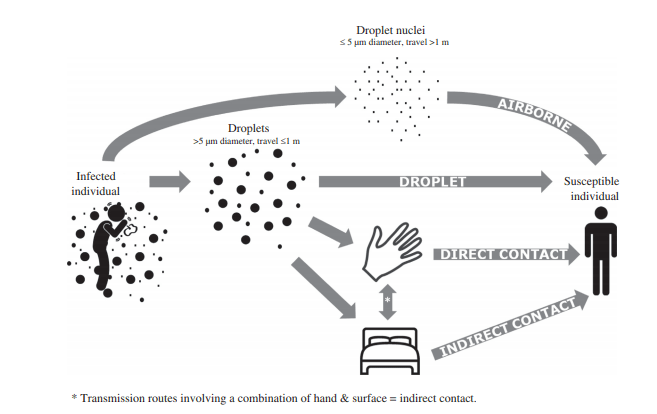
There are two transmission routes to consider for MERS-CoV: droplet / aerosol and contact / fomite. CDC recommends both airborne and contact isolation procedures to reflect these transmission routes. This involves placement of the patient in a negative pressure airborne infection isolation room, and the use of gloves, gowns, eye protection and N95 (FFP3) mask, and, of course, hand hygiene. PHE recommends a similar approach.
First and foremost, as a respiratory virus, inhalation of infected droplets is likely to be the most important transmission route. However, whilst not an ‘airborne’ virus (such as measles), aerosols can be generated by MERS-CoV patients that comprise small droplet nuclei that travel for long distances. A recent study of influenza suggests that the generation of aerosols is surprisingly common, to the extent that ‘living and breathing is an aerosol generating procedure’. Indeed, a recent study showed that a MERS-CoV aerosol diminished by only 7% over 10 minutes (compared with 95% for influenza). The use of an N95 (FFP3) mask will prevent direct inhalation of droplets / aerosols, and gloves, gowns and eye protection will prevent contact with mucous membranes and contamination of clothing or hands for subsequent nasal inoculation. But, if MERS-CoV aerosol is generated in the patient’s room (which seems likely), how long will it last and will the subsequent admission to the next room be at risk?
Let’s assume a patient sheds a MERS-CoV infectious aerosol of 6-log. I’m not aware of any infectious dose data for MERS-CoV yet, but for SARS-CoV it can be as low as <20 plaque forming units. Given the decay rate of 7% over 10 minutes, infectious aerosol above the infectious dose could be present after the discharge of the patient for a little under 26 hours! Even if the virus was shed at a lower titre, infectious aerosol times would still be considerable (Table). Could this be a job for automated room disinfection systems, which address both surface and airborne contamination? One such system, hydrogen peroxide vapour, has recently been shown to inactivate the SARS-CoV surrogate, TGEV.
| Shed titre |
Time to reach 20 virus particles |
| 1000000 |
26 hours |
| 100000 |
20 hours |
| 10000 |
15 hours |
| 1000 |
9 hours |
| 100 |
4 hours |
Table: Relationship between shed titre of MERS-CoV and time to reach 20 virus particles.
Whilst respiratory viruses are not that great at surviving on surfaces compared with C. difficile spores and some vegetative bacteria, they can survive long enough to bring contact / fomite transmission into play. A number of reviews have concluded that contact / fomite transmission is an important route for influenza and other respiratory viruses such as rhinovirus. The SARS-CoV and surrogates exhibit unusual survival properties compared with other respiratory viruses, with survival times often measured in days, weeks or even months. Recent data suggests that MERS-CoV shares this property, surviving for >2 days when dried onto hard surfaces compared with only a few hours for influenza tested in the same study. Fortunately, these enveloped viruses are inactivated rapidly by usual hospital disinfectants, so I can understand the CDC’s recommendation for standard environmental disinfection.
So, how to protect yourself and your patients? The answer is simple for direct patient care: wear your gown, gloves, goggles and N95 (FFP3) mask, and wash your hands! It’s simple in theory, compliance with these measures in practice is not as good as you may expect. Prof Seto published a study in the Lancet in 2003 about compliance with personal protective equipment (PPE) and hand hygiene during the SARS epidemic. Remarkably, even when caring for patients known to be infected with SARS, <30% of healthcare workers self-reported that they wore a mask, glove, gown and washed their hands as they should have done. And this was self-reported, so you’d expect there to be a bias towards compliance! Most importantly, none of the healthcare workers who complied with all four measures became infected.

Figure: Healthcare worker compliance with mask, glove, gown use, and hand washing during the SARS epidemic, stratified by those who became infected with SARS.
To summarise: how to protect you and your patients from MERS-CoV:
- Place patient in negative pressure airborne infection isolation room, where available.
- Wear the correct PPE when in the room (gloves, gown, N95 / FFP3 mask, goggles), and wash your hands.
- Pay attention to the potential for contaminated surfaces and air, particularly following the discharge of the patient.
- Oh, and if you go on holiday to Saudi Arabia, don’t kiss any camels!