During the first wave of COVID-19, we developed a ‘PPE Helper’ programme. This ward-based programme put PPE experts on the front line to spend time with staff to improve PPE knowledge, promote safe and effective use, and address staff anxiety. The programme was evaluated through a survey of staff views about PPE at the conclusion of the programme. This found that staff who had had contact with a PPE helper responded more positivity to questions about PPE and felt less PPE-related anxiety too.
Continue readingcoronavirus
There’s more to IPC & AMS than COVID-19
As parts of the world begin to contemplate life on the other side of this pandemic, it’s time to address that niggle in the back of our minds as our attention has been focussed on COVID-19: what’s been happening with those other HCAI and AMR issues that usually occupy our days (and nights)? This helpful opinion piece in ICHE discusses the impact of COVID-19 on our usual HCAI & AMR practice.
Explore the spread of COVID-19
COVID-19: Learning rapidly from an overwhelmed healthcare system in Bergamo, Italy
A very sobering piece published in NEJM Catalyst Innovations in Care Delivery (a new digital journal in the NEJM group) describes a catastrophic situation in a hospital in Bergamo, Italy, which has been overrun by COVID-19. We all have much to learn from this experience: about pandemic preparedness, response, and the key role of IPC at all stages of this pandemic.
COVID-19 – visualising the impact of social distancing
As we move through the gears of the response to the COVID-19 pandemic, the UK has entered lockdown – total social distancing. I’ve had many conversations with friends and family about what’s going on and why these extreme measures are necessary. I’ve pointed everybody who’s asked to the Imperial College London modelling, predicting a rapidly overwhelmed healthcare system if the trajectory of the UK epidemic doesn’t change. And pointed them in the direction of these rather cool visualisations of the logic behind social distancing (by cartoonist Toby Morris and microbiologist Siouxsie Wiles):

COVID-19: hello social distancing
The UK government yesterday announced a far-reaching package of social distancing measures to suppress the spread of COVID-19. These are based on some Imperial College London modelling work, published here. The model predicts that the UK approach to mitigate the impact of the UK epidemic would indeed reduce the overall number of people affected and those who die, but would still leave hundreds of thousands dead in an overwhelmed healthcare system. In contrast, a more intensive suppression approach would be effective in reversing the epidemic trend and keep the number of new cases to a low level – in the short term, at least.
Considering the role of environmental contamination in the spread of COVID-19
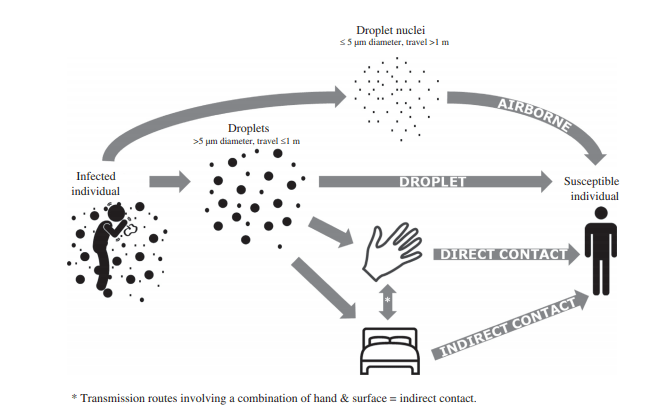
We know that respiratory viruses can be spread through droplets, occasionally aerosols, and contact routes (see Figure 1). But what is the relative importance of these transmission routes for the SARS-CoV-2 virus, which causes COVID-19? A new pre-print paper published yesterday provides evidence that the stability of the SARS-CoV-2 coronavirus is broadly comparable to the ‘original’ SARS coronavirus (SARS-CoV-1) on dry surfaces and in aerosols. This paper supports an important role for dry surface contamination and aerosols in the spread of SARS-CoV-2, and suggests that improved environmental persistence isn’t the key to the relative success of SARS-CoV-2 over SARS-CoV-1.
Figure 1: Transmission routes of respiratory viruses (from this review article).
Coronavirunoia
I guess it was inevitable really – the Coronavirus paranoia (or Coronavirunoia) is setting in!
I called my local GP today to get an appointment for my son…
Hello Novel Coronavirus
As I’m sure you’ve heard (unless you’ve been living under a rock), there’s something going on in China: a Novel Coronavirus has been identified, associated with an outbreak affecting 44 people (one of whom has died and a small number of whom are critically unwell) in Wuhan Providence, China. Here’s what we know so far:
Surface contamination and respiratory viruses with pandemic potential (SARS, MERS and influenza): an underestimated reservoir?
Most virologists would probably tell you that enveloped viruses are generally pretty fragile outside of their host and so wouldn’t survive for long on dry surfaces. They may well say “If you were talking about a non-enveloped virus (like norovirus) then, yes, it would probably survive on surfaces for quite a while. But enveloped viruses, no – you’d be lucky if it survived for more than a few hours.” But when I looked at the literature to investigate the potential for dry surface-mediated transmission of respiratory viruses with pandemic potential (SARS, MERS and influenza), the picture that emerged was quite different. These respiratory viruses can survive on dry surfaces for ages, and the contaminated environment may well be an underestimated reservoir for their transmission. This is summarised in a review published recently in the Journal of Hospital Infection.
