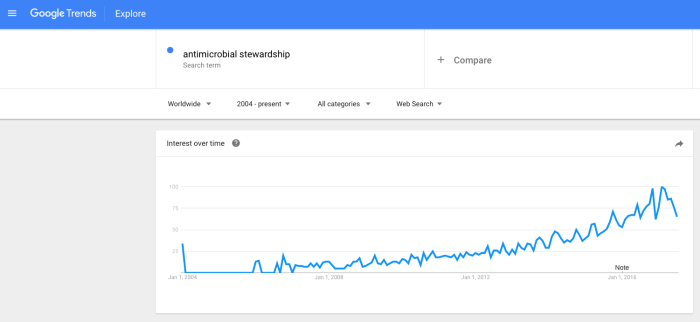
As we all enjoy Infection Prevention Week for 2025, I thought I’d take a look into the literature to see whether anybody has done some cost-effectiveness work for an IPC service as a whole. I came across this “Umbrella” review (i.e. a review of reviews!), which looks at the cost-effectiveness of interventions to tackle HCAI and AMR (to include IPC, AMS, diagnostic stewardship), and thought it was worth sharing. The bottom line: there’s a lot of cost-effectiveness evaluations for IPC interventions, most of which are cost-effective, but a bit of a gap around cost-effectiveness of the service as a whole.
Continue readingAMS
COVID-19 – what have we learned?
I did a talk at an IPC conference the other day trying to summarise what we’ve learned from the COVID-19 pandemic. You can see my slides here. I think (hope) we have learned a lot – and still have more to learn – about (in no particular order): PPE, transmission routes, testing and laboratory factors, vaccination, organizational transformation, guidelines and policy development, regulatory framework, outbreaks, non-COVID pathogens, antimicrobial stewardship, digital transformation, applied research, and the mental health of our workforce.

ESPAUR report to kick of WAAW 2021
It’s great to see the latest ESPAUR report published at the start of World Antibiotic Awareness Week 2021. There’s some good news in the report, but also some warning shots about our need to refocus on the risks attached to antimicrobial resistance as we move into the Covid endemic.

Setting our IPC priorities for the next 3-5 years
In honour of Infection Prevention and Control Week (#IIPW) 2021, I thought I put up a quick post based on a talk I did on Friday last week about the ‘Future of Healthcare and of Infection Prevention and Control’ (you can download my slides here). I used it as an opportunity to put across my strategic priorities for the next 3-5 years. And COVID-19 is bottom of the list – keep reading to find out why…
Continue readingThe role of IPC, vaccination, and OTC distribution in AMR
I had the privilege of chairing a session in the BSAC Spring Conference webinars yesterday about the role of IPC, vaccination, and OTC distribution in AMR. The session had a talk from Professor Andreas Voss on IPC as a cornerstone of successful stewardship, Dr Elizabeth Klemm on prevention through vaccination, and Dr Abdul Ghafur on community pharmacy and the challenge of over-the-counter (OTC) distribution.
Continue readingThere’s more to IPC & AMS than COVID-19
As parts of the world begin to contemplate life on the other side of this pandemic, it’s time to address that niggle in the back of our minds as our attention has been focussed on COVID-19: what’s been happening with those other HCAI and AMR issues that usually occupy our days (and nights)? This helpful opinion piece in ICHE discusses the impact of COVID-19 on our usual HCAI & AMR practice.
ESPAUR 2019: a snazzy facelift
The 2019 edition of the ESPAUR report has recently been published, including data up to and including 2018. The report is an excellent read – here’s a few summary points.
- There’s a series of lovely infographics at the start of the report. I gave myself a challenge: to select the one infographic that told the story of the report. I toyed with the one about a small but increasing number of CPE BSIs (aghhhhh!), and the stark grave-stone themed image of mortality related to carbapenemase-producers, but ended up with this one: alarmingly, the rate of BSI for the seven priority bacterial pathogens rose 22% between 2014 and 2018 to 145 per 100,000 population. (Around half of these were coli). And there’s a certain inexorability about the antimicrobial resistance trends included in this report, with a 32% increase in AMR BSIs comparing 2014 to 2018.
Figure: Trends in BSIs (blue line) and AMR BSIs (green line).
- There were more than 60k antibiotic resistant severe infections in 2018, <150 per day.
- Confirmed CPEs have topped 4k (but this is a gross underestimate of true prevalence). The report makes the case that the rarity of CPE BSIs (142 reported nationally) represents a success of prevention. This is probably true if we compare across the pond and towards the southern reaches of Europe. But difficult to be sure without a control (i.e. what would have happened without the national initiatives etc)? Also, reporting of CPE BSIs to PHE is voluntary and not mandatory, so there will be some degree of under-reporting.
- Related to this, only 50% of diagnostic labs have introduced methods to detect CPE locally. Which links closely with the change in surveillance system for CPEs going forwards – rather than manual voluntary reporting, locally confirmed CPEs will be reported automatically to PHE. However, if only 50% of diagnostic labs have appropriate methods, we’ll still end up under-reporting (but it will be more a more accurate picture than the current process provides).
- 30 day all-cause mortality of invasive CPE infections is 24% (along with the arresting gravestone-themed infographic)! Not sure how helpful it is to make a big point based on unadjusted mortality data…
- Overall consumption of antibiotics continues to decline. Consumption fell from 20 to 18 DDDs per 1,000 population per day between 2014 and 2018. However, consumption increased by 3% in hospitals over this period.
- There’s a nice section on Candida auris
- ESPAUR reports some good work and outcomes related to training, education, and awareness (e.g. Keep Antibiotics Working and Antibiotic Guardian).
- What a wonderful resource the AMR Fingertips module is: automated data from >90% of NHS laboratories on a range of AMR indicators at our…ahem…fingertips. I am one of the 15k users over the past three years. (As an aside, the volume of traffic is fairly low by popular website standards – but I guess it is somewhat niche!)
ESPAUR is a fantastic resource – it seems that this is the last ESPAUR report related to the UK AMR Strategy from 2013-2018, but I’m confident that ESPAUR will continue to report the successes and challenges of implementing the new five year action plan (from 2019-2024).
Nine decades of antibiotics: a story with two endings…
I did a talk today in Portugal covering the nine decades since Fleming discovered the effects of Penicillium sp. in 1928. I thought it would be interesting to have two endings to the talk: an upbeat one, and a doomsday one.
Online HCAI / IPC / AMR / AMS / training resources
I am on the hunt for some free online training resources for HCAI / IPC / AMR / AMS / IPC, at a basic, intermediate, or advanced level. Here’s a summary of what I’ve unearthed so far.
Effective stewardship: less antibiotic use and more hand hygiene
Rossana Rosa (bio below) writes a guest post, reflecting on this recent review and meta-analysis on the effectiveness of antimicrobial stewardship (AMS) programmes…
The first reports on the effects of Antimicrobial Stewardship Programmess date back to the mid-90s, and the interest in them has taken off in the past decade.