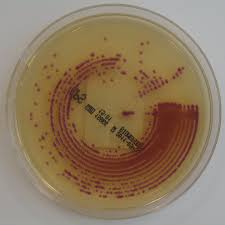
The emergence of CPE (and carbapenem-resistance in other Gram-negative bacteria) has forced us to reach to the dusty old antibiotic shelf to revive the clinical use of older agents with activity against Gram-negative bacteria, principally colistin. Colistin isn’t perfect by any means – it has poor tissue penetration compared with the carbapenems, and is associated with nephrotoxicity (although the high levels of nephrotoxicity in the older medical literature has not been reported due to better management of the drug). Furthermore, resistance has already been reported. To date – this has been mutational resistance, which does not have the capacity to spread horizontally. It was only a matter of time before a colistin resistance gene mobilised.
Antibiotic Awareness: background and links
European Survey of Carbapenemase-Producing Enterobacteriaceae (EuSCAPE) project
The EuSCAPE project aimed to improve understanding of the occurrence and spread of CPE. LINK

About European Antibiotic Awareness Day
European Antibiotic Awareness Day is a European health initiative coordinated by ECDC which aims to provide a platform and support for national campaigns on the prudent use of antibiotics. Each year across Europe, the European Antibiotic Awareness Day is marked by national campaigns on the prudent use of antibiotics during the week of 18 November. Prudent use means only using antibiotics when they are needed, with the correct dose, dosage intervals and duration of the course. Follow the European Antibiotic Awareness Day: #EAAD. http://antibiotic.ecdc.europa.eu
About World Antibiotic Awareness Week
The World Health Organization is leading a global campaign for the first World Antibiotic Awareness Week with the slogan “Antibiotics: Handle with Care”. The campaign calls on individuals, governments and health and agriculture professionals to take action to address this urgent health problem. The first World Antibiotic Awareness Week will take place on 16-22 November. Follow the World Antibiotic Awareness Week: #AntibioticResistance. www.who.int/drugresistance.
Continue reading
European Antibiotic Awareness Day 2015: ESPAUR report highlights progress and challenges
For those of you who have had your head in a hole all week, you may not be aware that today is European Antibiotic Awareness Day, which coincides with Global Antibiotic Awareness Week. The antibiotic stewards amongst us (which should really be all of us!) have launched many and varied campaigns to highlight the need to handle antibiotics, our ‘miracle drugs’, with care (see Andreas’ 30-second-antibiotics-myth-buster-survey, for example).
The 30-Second-Questionnaire: Antibiotic Myth Buster
Here we are again, the year flew by and it’s time for Antibiotic Awareness Day/Week. This time around, I will spend my time in a call-center, answering questions of concerned citizens/ex-patients in Germany. Smart idea of a friend in the German public health service and probably smarter than doing what we usually do: organize a meeting, ask all our colleagues to come, and preach to our own community.
While I believe that there is no ID or Clin Micro person left that is not convinced of the importance of saving our miracle drugs (Australian campaign), I know that I will get questions I can’t answer, or at least, don’t know if my answers are truly true.
Here it goes, my antibiotic conundrum that could be classified as “Antibiotic Myth”:
Is it true that I have to finish my antibiotic treatment as prescribed?
Will “too short” lead to antimicrobial resistance, or is it the “too long”? My guess, 99% of the professionals will answer this question by releasing an avalanche of questions, regarding the bug, the host and the site of infection, but I have to insist on a simple “yes” or “no”. Sorry, but those are the rules of the “30-Second-Questionnaire” and you can’t argue the rules.
Thus here is my request. Follow the link to the questionnaire, take 30 seconds to answer the question (and 4 others) and email, twitter, blog or use any kind of communication you can think of to forward it to your friends and family. I promise, I will post the outcome right here, a week or two later.
UK guidelines for the control of multidrug-resistant Gram-negative bacteria
The UK guidelines for the prevention and control of multidrug-resistant Gram-negative bacteria (MDR-GNB) are published this week. It’s useful that the publication of these guidelines coincides with Antibiotic Awareness Week because MDR-GNB are brining us ever closer to the end of antibiotics. Although the guidelines don’t cover the treatment of MDR-GNB (this will be addressed in a forthcoming guideline), these highly resistant MDR-GNB leave few therapeutic options. Even when they remain susceptible to some antibiotics, these antibiotics are not front-line antibiotics for a reason (including poor tissue penetration and side effects). Furthermore, we are already seeing resistance to last-line (aka end of the golden-antibiotic-road) antibiotics e.g. colistin. Therefore, the old adage that ‘prevention is better than cure’ has never been so true!
Appraising the options for detecting carbapenemase-producing organisms
Carbapenemase-producing organisms (including CPE) present important clinical challenges: the “triple threat” of high levels of antibiotic resistance, virulence, and potential for rapid spread (locally, regionally, nationally, and globally)! However, these organisms somewhat ironically also present challenges to detection in the clinical laboratory. You’d expect that since these organisms are so important clinically they’d be dead easy to detect in the clinical lab – but this isn’t the case.
A comprehensive review published in Clinical Microbiology Reviews provides an overview of the diagnostic approaches to detect carbapenemase producers in the clinical lab. Figures 6 and 7 of the review provide a useful overview of the two broad approaches you could take: culturing organisms on agar plates, or using nucleic acid amplification techniques (NAAT – most commonly PCR) directly from a rectal swab.
Cost of CDI – New estimate, but how accurate?
 To be honest I’m a bit fed up with quoting the £4000 per CDI case that was calculated by Mark Wilcox and colleagues back in 19 0 plonk (1996 to be exact) and so I was quite excited to stumble across a new estimate from Merseyside whilst browsing ‘Value in Health‘, one of my usual reads. Well, possibly not.. although perhaps it should be – and it does support open access.
To be honest I’m a bit fed up with quoting the £4000 per CDI case that was calculated by Mark Wilcox and colleagues back in 19 0 plonk (1996 to be exact) and so I was quite excited to stumble across a new estimate from Merseyside whilst browsing ‘Value in Health‘, one of my usual reads. Well, possibly not.. although perhaps it should be – and it does support open access.
Nakamura and colleagues presented an abstract at the 18th International Society for Pharmacoeconomics and Outcomes Research (ISPOR) meeting and have calculated the mean extra cost of a patient with CDI to be £10,956.82, although as the authors point out, how much of this is attributable to the extra cost of CDI rather than the multiple co-morbidities that likely contributed to the infection leading to the antibiotic treatment, which led to the CDI continues to elude us. The authors are continuing to work on this and I await their final findings with interest, however for now I’ll settle for £11,000 per case as opposed to the 1996 figure of £4000 (data collected in 1995) and is probably more realistic than just allowing for inflation that has averaged at 2.8% pa, which would have made it £6868. As we know (well all of us apart from the Treasury), health inflation is way ahead of normal financial indicators.
Influenza among afebrile and vaccinated HCWs
Picture: gerardnadal.com
Influenza is considered to contribute to the morbidity and mortality of our patients and during the flu season, some estimate that as many as 1 in 5 patients contract nosocomial influenza; via infected HCWs.
After having had close and personal experience with influenza last season I do have a better understanding for some things.
- You don’t want influenza if you can avoid it!
- I fully understand while you wish your worst enemies to have an inflammation of their pleura (Dutch saying: “Go and have pleuritis”) – it really, really hurts – A LOT.
- Flu vaccination programs for HCWs and guidelines preventing febrile HCWs to work may be a pretty smart idea! Or not?
In a recent study, Ridgway et al. had a look at the validity of “febrile” as an indicator of having influenza. After screening 449 HCWs with respiratory symptoms, they found a total of 41 (9.1%) with proven influenza. Only half of the HCWs actually were febrile, with no significant differences between vaccinated and non-vaccinated HCWs.
Thus, while we should continue to vaccinate our HCWs (in my opinion, not part of the article) and hope for a match of the vaccine with the circulating virus, the practice to only look for influenza in febrile HCWs needs to be reconsidered.
Reference
Ridgway JP, Bartlett AH, Garcia-Houchins S, Cariño S, Enriquez A, Marrs R, Perez C, Shah M, Guenette C, Mosakowski S, Beavis KG, Landon E. Influenza among afebrile and vaccinated healthcare workers. Clin Infect Dis. 2015 Jun 1;60(11):1591-5.
The room lottery: why your hospital room can make you sick
In this era of increasing patient choice, let’s imagine you were offered the choice between two identical looking hospital rooms. Your chances of picking up a multidrug-resistant organism (MDRO) are approximately doubled if you choose the wrong room. But you have no way of knowing which room is safest.
So what explains this lottery? The key information you have not been told is the MDRO status of the previous room occupants. One of the rooms was previously occupied by a patient with C. difficile, and if you choose this room, your risk of developing C. difficile infection doubles. And it’s not just C. difficile – this same association has been demonstrated for MRSA, VRE, Acinetobacter baumannii and Pseudomonas aeruginosa. Underpinning this association is the uncomfortable fact that cleaning and disinfection applied at the time of patient discharge is simply not good enough to protect the incoming patient.
Norovirus – The organisation’s IPC ‘Canary’
 It’s the most Chunderful time of the year (or maybe not). The Norovirus ‘season’ will still be on us and a few points are well worth reflecting on. A recent systematic review of Norovirus risk in high and middle-income countries asserts that there may be as many as 12.5 million infections annually these countries alone, with possibly as many as 2.2 million outpatient visits related to the illness. Personally I have always liked having a bit of norovirus around. Keeps the staff on their toes and gives a good indicator of how IPC is really being performed rather than another set of 99% compliant hand hygiene audits.
It’s the most Chunderful time of the year (or maybe not). The Norovirus ‘season’ will still be on us and a few points are well worth reflecting on. A recent systematic review of Norovirus risk in high and middle-income countries asserts that there may be as many as 12.5 million infections annually these countries alone, with possibly as many as 2.2 million outpatient visits related to the illness. Personally I have always liked having a bit of norovirus around. Keeps the staff on their toes and gives a good indicator of how IPC is really being performed rather than another set of 99% compliant hand hygiene audits.