 We often see those tasked with finding suitable isolation facilities counting down to when precaustions can be discontinued and the ’48 hours clear’ of symptoms of loose stools or vomiting has almost become one of the most welcome statements heard in healthcare settings. No more contact precautions, no more disinfectants sloshing around, normality beckons.. Or should it? Continue reading
We often see those tasked with finding suitable isolation facilities counting down to when precaustions can be discontinued and the ’48 hours clear’ of symptoms of loose stools or vomiting has almost become one of the most welcome statements heard in healthcare settings. No more contact precautions, no more disinfectants sloshing around, normality beckons.. Or should it? Continue reading
CDI
Crapsules part 2
How do you like your crap? Fresh or frozen?
 Since Jon’s post on crapsules is one of the most favorite on the blog, I assumed that many of you might enjoy a sequel.
Since Jon’s post on crapsules is one of the most favorite on the blog, I assumed that many of you might enjoy a sequel.
Clostridium difficile infections (CDI), most certainly after the emergence of hypervirulent strains at the beginning of this millennium, have become a major cause of morbidity and mortality in hospital and (to a lesser degree) community patients. One in four patients will suffer from recurrent CDI and treatment options are limited. Consequently, fecal microbiota transplantation (FMT) has become a valuable alternative, but is not readily available. Using frozen FMT would make the logistics far easier and finally something frozen seems to be as good as fresh, according to this JAMA study!
Molecular diagnostics for C. difficile infection: too much of a good thing?
A study in JAMA Internal Medicine suggests that we may be ‘overdiagnosising’ C. difficile in this era of molecular diagnostics. The researchers from California grouped the 1416 patients tested for C. difficile into three groups: Tox+/PCR+ (9%), Tox-/PCR+ (11%), and Tox-/PCR+ (79%) (see Figure). Perhaps unsurprisingly, compared with Tox+/PCR+ cases, Tox-/PCR+ cases had lower bacterial load, less prior antibiotic exposure, less faecal inflammation, a shorter duration of diarrhoea, were less likely to suffer complications, and were less likely to die within 30 days. Perhaps even more importantly, patients with Tox-/PCR+ were pretty much identical to patients with Tox-/PCR- specimens in all of these metrics. In short: these patients had C. difficile in their gut, but they did not have C. difficile infection. The key message here is that we should not be treating patients who are C. difficile “positive” by molecular tests only.
We need to work together to reduce CRE and other pathogens
Some fascinating modelling from the CDC Vital Signs programme suggests that a co-ordinated, multi-facilitiy approach will be much more effective than each hospital doing its own prevention interventions.
The team first estimated the burden of key infections in the US: CRE, multi-resistant P. aeruginosa, invasive MRSA and CDI combined were responsible for 310,000 infections in 2011, which would increase 10% to 340,000 over 5 years. However, with an ‘aggressive’ national intervention, this could be reduced to below 200,000 by 2019. It would be a huge undertaking to implement and co-ordinate a national campaign in the US, where there is so much heterogeneity in the way that hospitals are structured and funded. But if anybody can do it, the CDC can!
Fidaxomicin reduces C. difficile environmental contamination
It is well-established that fidaxomicin reduces the recurrence rate of C. difficile infection (CDI), but this study from my old research group at GSTT / KCL is the first to evaluate the impact of treatment with fidaxomicin on environmental contamination. The bottom line is that patients treated with fidaxomicin had less C. difficile contamination than patients treated with vancomycin / metronidazole.
In total, the rooms of 38 / 66 (57.6%) patients treated with metronidazole / vancomycin had one or more positive environmental cultures compared with 25 / 68 (36.8%) patients treated with fidaxomicin (P = 0.02). Similarly, when considering all of the sampled environmental sites (four per room), 68 / 264 (25.8%) were positive in patients treated with metronidazole / vancomycin compared with 47 / 272 (17.3%) in patients treated with fidaxomicin (P = 0.02) (see Figure below).
Figure: Environmental contamination with C. difficile in the rooms of patients treated with fidaxomicin vs. vancomycin / metronidazole.
‘Crapsules’: the cure for Cdiff and more
I gave a talk today at a Pint of Science event entitled “Crapsules: the cure for Cdiff and more”. You can download my slides here. Cdiff infection (CDI) is a nasty disease, usually occurring in those who have taken antibiotics in hospital. It’s characterised by frequent loose stools (often 5 or more movements per day) and frequent recurrence. Around 15-35% of patients with CDI will have a repeat episode. The mainstay treatment for recurrent CDI is antibiotics but the cure rate is poor at around 30%. Remarkably a ‘faecal microbiota transplantation’ (FMT) is way more effective, with a cure rate in excess of 90%.
How big is C. difficile infection in the USA?
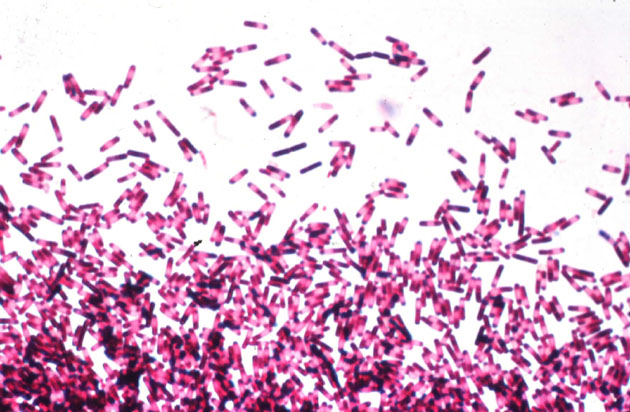 The New England Journal of Medicine recently published an article evaluating the burden of CDI in the USA. The huge CDC-led initiative collected data from 10 geographically distinct regions, identifying more than 15,000 cases. Around two-thirds of cases were classified as healthcare-associated (although only 25% were hospital-onset). This means that, prima facie, a third of CDI cases were community-associated. I find this proportion difficult to believe: I strongly suspect that many of these cases would have had healthcare-associated risk factors if the team were able to look hard enough. For example, they used a fairly standard 12 week look-back period to evaluate previous hospitalisation, but how would the data look if they’d used 12 months? Also, it’s usually only possible to evaluate previous hospitalisation in a single healthcare system, but many patients commute between various healthcare systems. The authors acknowledge in the discussion that this designation of “community-acquired” may be inaccurate based on the finding from a previous study whether healthcare-associated risk factors were identified in most patients, but only be a detailed phone interview.
The New England Journal of Medicine recently published an article evaluating the burden of CDI in the USA. The huge CDC-led initiative collected data from 10 geographically distinct regions, identifying more than 15,000 cases. Around two-thirds of cases were classified as healthcare-associated (although only 25% were hospital-onset). This means that, prima facie, a third of CDI cases were community-associated. I find this proportion difficult to believe: I strongly suspect that many of these cases would have had healthcare-associated risk factors if the team were able to look hard enough. For example, they used a fairly standard 12 week look-back period to evaluate previous hospitalisation, but how would the data look if they’d used 12 months? Also, it’s usually only possible to evaluate previous hospitalisation in a single healthcare system, but many patients commute between various healthcare systems. The authors acknowledge in the discussion that this designation of “community-acquired” may be inaccurate based on the finding from a previous study whether healthcare-associated risk factors were identified in most patients, but only be a detailed phone interview.
Scaling up from the figures from the 10 regions, national estimates were around 500,000 cases and 29,000 deaths due to CDI per annum in the US. This estimate is approximately double previous estimates for the national CDI burden in the USA, probably reflecting the adoption of molecular methods for the detection of CDI. This scaling up included an interesting statistical adjustment to see how prevalence varied depending on how many sites use sensitive molecular methods to detect CDI.
A sub-study included the culture of C. difficile from 1625 patients. More than 15% of stool specimens from patients diagnosed as CDI failed to grow C. difficile, probably illustrating the limitations of culture methods more than anything else. NAP1 (027) represented around half of cases, and was significantly more common in healthcare-associated CDI. I think it’s fair to say that the initial fears that NAP1 was a super-strain have been allayed by the fact that it’s now so common and there hasn’t been a surge in CDI mortality.
Finally, around 21% of healthcare-associated cases suffered at least one recurrence. Thus, there is a real need to the roll out of the uber successful faecal microbiota transplantation for recurrent CDI. In fact, there should be around 70,000 faecal microbiota transplantations each year in the US right now (500,000 x 0.66 x 0.21); I suspect there are far fewer.
Over the top and into the trenches
 After 12 years working for Bioquell (and part-time at Guy’s and St. Thomas’ / King’s College London since commencing my PhD in 2005), it’s time for me to move onto pastures new. Next week I’ll start working in a leadership role in Infection Prevention and Control at Imperial College NHS Trust in London. It’s a very exciting move for me and I can’t wait to get going. I thought that now would be a good time to reflect on the water under the bridge of the last decade or so (and I hope you’ll forgive my self-indulgence).
After 12 years working for Bioquell (and part-time at Guy’s and St. Thomas’ / King’s College London since commencing my PhD in 2005), it’s time for me to move onto pastures new. Next week I’ll start working in a leadership role in Infection Prevention and Control at Imperial College NHS Trust in London. It’s a very exciting move for me and I can’t wait to get going. I thought that now would be a good time to reflect on the water under the bridge of the last decade or so (and I hope you’ll forgive my self-indulgence).
Over the last decade, the rate of MRSA and C. difficile infection (CDI) in the UK have fallen dramatically.1,2 At the peak of the MRSA epidemic in the early 2000s, there were more than 2000 MRSA bloodstream infections per quarter in England; now there are 10-fold less.2 It’s not certain how this has been achieved, but a combination of factors, including increased governmental focus, are likely responsible. Whilst MRSA is now rare in the UK this is not the case in other European countries and in many other parts of the world, where MRSA remains common.3
In recent years, a new and more troublesome bacterial threat has emerged: carbapenem-resistant Enterobacteriaceae (CRE).4 CRE present the “triple threat” of high levels of antibiotic resistance (including pan-drug resistant strains against which no antibiotics are left), severe clinical consequences (around half of patients with a CRE bloodstream infection will die), and the potential for rapid regional and national spread (illustrated by national outbreaks in Italy, Greece and Israel).4-6 CRE have been described as “nightmare bacteria” by the US CDC and have prompted unprecedented action from CDC, Public Health England (PHE) and other public health agencies, including a national Patient Safety Alert and a letter to all hospital Chief Executives in the UK to ensure that new CRE guidelines are implemented.7,8
Journal Roundup November 2014: Journal Roundup: Ebola (again), The rise (and rise) and fall of MRDOs & Infection Prevention 2014
This month’s Roundup, as ever freely available on the Journal of Hospital Infection website, showcases some of the useful data emerging from the field of the ongoing outbreak of Ebola in West Africa. For example, emerging data suggests that the R0 (basic reproductive number) of Ebola is around 2, meaning that two transmissions will occur from every case. This means that Ebola is not massively transmissible compared with other infectious diseases – but this hasn’t stopped it increasing more or less exponentially in parts of West Africa!
Some interesting studies on the increasing or decreasing prevalence of MDROs are also covered in the Roundup. For example, one study reported a worrying doubling of the rate of CDI in the USA, whereas another study reports impressive reductions in S. aureus bacteraemia in Australia.
The Roundup includes a brief overview of the Infection Prevention 2014 conference, covered in more detail in a previous post in this blog, and finally, features Catherine Makison-Booth’s brilliant Vomiting Larry (pictured below)!
As ever, I’d be delighted to receive your feedback as to how the Roundup should evolve.
Summer 2014 Update
It’s been another busy quarter on the blog, with some updates from ECCMID and APIC, the inaugural ‘Journal Roundup’ plus a few key studies.
- ESCMID MDR-GNR guidelines (Published 2nd July 2014)
- Inaugural ‘Journal Roundup’ (June 2014) (Published 26th June 2014)
- What works to control antibiotic-resistant bacteria in the ICU? A two-for-the-price-of-one study (Published 17th June 2014)
- Highlights from APIC 2014 (Published 9th June 2014)
- Which transmission route is most important for influenza? (Published 4th June 2014)
- MERS-CoV: a survival guide for you and your patients (Published 28th May 2014)
- Perspectives from ECCMID 2014: the box set (Published 21st May 2014)
- Perspective from ECCMID Part IV: We need to stop polluting our planet with antibiotics (Published 20th May 2014)
- Perspective from ECCMID Part III: CDI synthetic “repoopulation” (bacteriotherapy) closer than you think & “CA-CDI” still pie in the sky (Published 19th May 2014)
- Perspective from ECCMID 2014 Part II: What to do about MDR-GNR? (Published 16th may 2014)
- Perspective from ECCMID 2014 Part I: a voice against ‘selective’ digestive decontamination (SDD) (Published 15th May 2014)
- What does lab diagnosis of MDR-GNR have to do with SURFing? (Published 9th May 2014)
- Chronic wound? No problem – a splash of oxygen peroxide should do the trick (Published 7th May 2014)
- How much Clostridium difficile infection is hospital-acquired? Part II (published 29th April 2014)
- APIC New England 2014 Conference Report: ‘The how, when, & where of C. diff – can you “C” the difference?’ (Published 25th April 2014)
- IFIC 2013 Conference Report (Published 17th April 2014)
Please keep your responses coming – and let me know if you’d like to contribute a guest blog!
Photo: ‘Summer’ by Matteo Angelino.




