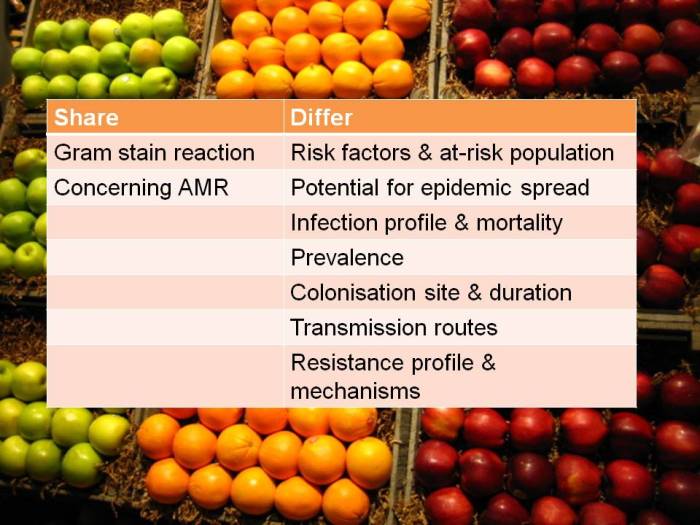
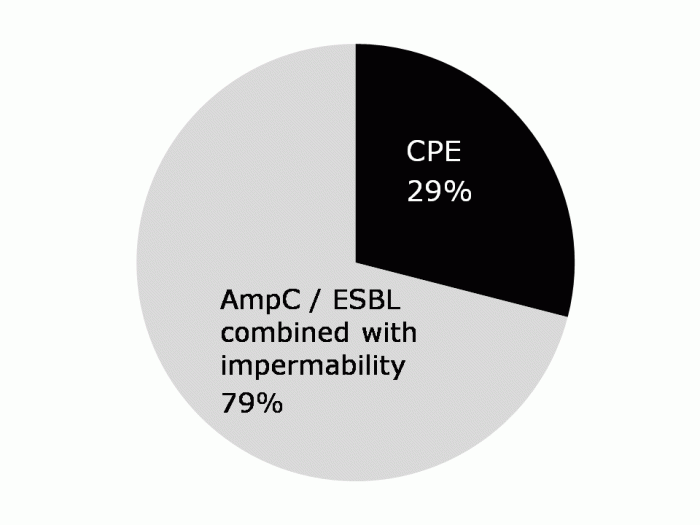
Carbapenem-resistant Enterobacteriaceae (CRE) present unique challenges to infection prevention and control. Firstly, unlike MRSA and C. difficile, CRE can be caused by multiple genetic determinants (typically KPC, VIM, NDM and OXA-48 types) in multiple species. The combination of resistance determinants and species may have distinct characteristics with transmission and control implications. Further, there is a larger pool of resistance determinants for horizontal transfer. Secondly, CRE colonize the gastrointestinal tract, so deconlonization therapy is likely to be limited to suppressing the amount of CRE in the gut; elimination of the carrier state, which has been a mainstay of prevention and control interventions for MRSA, seems unlikely. Thirdly, pan-drug resistant CRE has already been reported and the pipeline for new agents is virtually empty, meaning that effective therapeutic options will be increasingly limited.
Carbapenem-resistant Enterobacteriaceae (CRE) present unique challenges to infection prevention and control. Firstly, unlike MRSA and C. difficile, CRE can be caused by multiple genetic determinants (typically KPC, VIM, NDM and OXA-48 types) in multiple species. The combination of resistance determinants and species may have distinct characteristics with transmission and control implications. Further, there is a larger pool of resistance determinants for horizontal transfer. Secondly, CRE colonize the gastrointestinal tract, so deconlonization therapy is likely to be limited to suppressing the amount of CRE in the gut; elimination of the carrier state, which has been a mainstay of prevention and control interventions for MRSA, seems unlikely. Thirdly, pan-drug resistant CRE has already been reported and the pipeline for new agents is virtually empty, meaning that effective therapeutic options will be increasingly limited.
Data from EARS-Net suggests that the prevalence of CRE among bloodstream infections is low in most parts of Europe, with a gradual year-on-year increase. In Greece though, rates are exceptionally high, with the proportion of K. pneumoniae invasive isolates resistant to carbapenems increasing from 27.8% in 2005 to 68.2% in 2011. Also, rates in Cyprus are on the rise with 0% reported in 2006 up to to 15.7% in 2011. In the UK, rates of carbapenem resistance amongst K. pneumoniae have remained consistently <1% for the same period. Disturbingly, there has been a dramatic increase in the prevalence of carbapenem-resistant K. pneumoniae in the last few years in Italy, from 1% in 2009 to 15% in 2010 to 27% in 2011.
 [Chart: Changes in proportion of carbapenem resistance in K. pneumoniae invasive isolates. Data from EARS-Net.]
[Chart: Changes in proportion of carbapenem resistance in K. pneumoniae invasive isolates. Data from EARS-Net.]
A recent Eurosurveillance article reports a national survey of carbapenem resistance in Italy. 25 laboratories across the country participated and analyzed all consecutive, non-duplicate Enterobacteriaceae clinical isolates for six weeks in mid 2011. A total of 7,154 isolates were collected from inpatients and 6,595 isolates from outpatients. The highlight findings are:
- 3.5% of inpatient isolates and 0.3% of outpatient isolates carbapenem resistant.
- Carbapenem-resistant K. pneumoniae (CR-KP) the most problematic CRE, with 11.9% of K. pneumoniae isolates CR.
- Substantial geographical variation in resistance rate, ranging from 0 to 33% for CR-KP.
- KPC accounted for 90% of CRE enzymes; one CR-KPC clone predominated (CC-258).
- Resistance to other agents was common amongst KPC-producing K. pneumoniae; 22% were resistant/non-susceptible to colistin, 21% to tigecycline and 16% to gentamicin; 1.5% were non-susceptible to all three.
This study raises several challenging questions. What do you do with a CR-KP isolate causing an infection that is also resistant to colistin, gentamicin and tigecycline? This seems to be true pan-resistance, with supportive care the only option.
Why is KP the outstanding CRE, specifically the CC-258 clone? What does it have that the other CRE lack? K. pneumoniae seems to survive better on surfaces that other Enterobacteriaceae, and has been associated with more hospital outbreaks than other Enterobacteriaceae historically. However, further research is required to answer this question.
Can the worrying trend of CRE in Italy be reversed? An aggressive, national intervention was successful in Israel, and there are some local success stories in Italy. However, brining the situation under control in Italy will require an aggressive, national programme that must be implemented immediately. Otherwise, CR-KP will quickly become endemic and probably impossible to bring under control.
The authors should be complimented for performing a timely study, but I do wonder whether the situation is considerably worse now, 12 months later, given the shape of the national epi curve.
Citation: Giani T, Pini B, Arena F, Conte V, Bracco S, Migliavacca R, the AMCLI-CRE Survey Participants, Pantosti A, Pagani L, Luzzaro F, Rossolini GM. Epidemic diffusion of KPC carbapenemase-producing Klebsiella pneumoniae in Italy: results of the first countrywide survey, 15 May to 30 June 2011. Euro Surveill 2013;18(22):pii=20489.
Image permission: Original image obtained from http://www.freestock.ca.