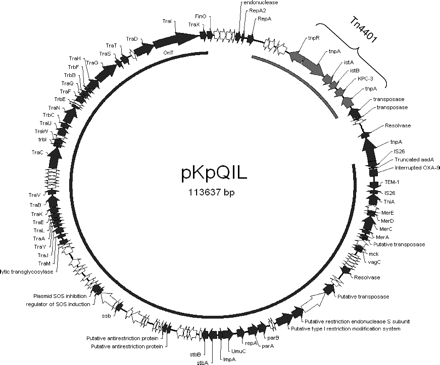
A genomic study of 44 isolates of CPE from various species identified between 2008 and 2010, mainly from the Northwest of England, has concluded that plasmids played a key role in the early dissemination of CPE.
The antibiotic course has had its day? (part 2)
British colleagues found no scientific evidence for “completing your course of antibiotics”. Nothing new, but in the absence of competing news (the White House has become a daily soap) they opened Pandoras’ box for the lay press, with patients being recommended to stop their antibiotics, whenever they want. The birth of yet another inconvenient truth, as we cannot translate our knowledge into daily medical practice, and patients get even more confused. The good news: a new research agenda. Continue reading
A health economist’s guide to the AMS galaxy
Guest blogger Nikki Naylor (bio below) has written this post about a recent review on the cost-effectiveness of antimicrobial stewardship…
I’ll start this blog post off with a promise – I promise not to use any equations or unnecessarily complex terms that just describe logical concepts (something us economists do like to do on occasion). In return, I hope that you will see past the standard and not-to-exhilarating conclusion of “more evidence is needed” and see some of the more useful messages that sit within this recent review that we have published.
The antibiotic course has had its day?

In a recent BMJ article, Llewelyn et al. argue that the old dogma of completing a prescribed course of antibiotics to prevent antibiotic-resistance is a myth, not based on evidence. Actually the opposite, namely taking antibiotics for longer than necessary, increases the risk of resistance.
While I love breaking down old dogmas (we actually had a poll on this topic some time back), many of today’s papers in the Netherlands (and I am pretty sure elsewhere, too) misinterpret the study, by slaughtering the message to patients to “always complete the full prescription”. One of the Netherlands most influential newspapers the Volkskrant, already wrote: “Finishing antibiotic course? Nonsense.”
SSIs – time to de-invest in laminar flow?
Laminar flow is a very embedded technology for the prevention of SSI in some types of surgery (especially hip and knee arthroplasty). However, it seems from a recent Lancet ID review that this widely adopted practice is way ahead of the evidence supporting it: the bottom line finding of the review is we should stop wasting time and money on laminar flow theatres for some procedures, and focus on basic prevention initiatives (especially getting antibiotic prophylaxis right) in all surgical categories.
More coffee = less AMR?
This one is for lovers of the brown stuff (no, the other brown stuff). I was taken by a large impressive epi study published in AIM showing that coffee consumption is associated with reduced all-cause mortality. Part of this seems to be tied up in a modified inflammatory response. Whilst the study didn’t mention infection specifically, clearly infection and inflammation are closely linked. So, this got me to asking whether anybody has looked at coffee consumption and infection / AMR outcomes?
Sloppy science & good read
I’m packing for vacation. The book that I will NOT pack is: Rigor Mortis, how sloppy science creates worthless cures, crushes hope and wastes billions by Richard Harris. I read it already two times, and anyone interested in science, or trying to deliver a piece of it once in a while, should read it. It makes you realise what we do, what we publish and what we read. And then, it makes you humble (or sad, or furious, or happy). Continue reading
Agent Orange in spinal surgery
This week I learned from an orthopaedic surgeon that randomized trials were something that could be of use in “pharmaceutical sciences”, but that it is well-known that in the “surgical science” retrospective analyses are better for deriving evidence. We came to this when discussing the benefits of powdered vancomycin in the wounds of spinal surgery. Apparently this is something “all spinal orthopaedics do”, because it works so good. Continue reading
Contact Precautions for Endemic MRSA and VRE
 by Andreas Voss and Eli Perencevich,
by Andreas Voss and Eli Perencevich,
intentionally posted on “Reflections” and “Controversies” at the same time as a reaction to the JAMA Viewpoint by Morgan, Wenzel & Bearman
During the recent ICPIC 2017 and a pre-meeting think tank, the sense and non-sense of RCTs looking at various infection control measures was a major point of discussion during many sessions. Data from well-designed quasi-experimental studies, epidemiological evidence, and logic seems to vanish, whenever a new RCT is published, even if the results are not applicable to situations that are non-endemic, have higher or lower compliance with the preventive measures in question, or whether the intended measures were actually applied within the intended patient group. Some studies seem to assume that the transmission during the first days of admission are of no consequence. Others assume that given endemicity and a high patient load, the intended measures such as single-room isolation can’t be applied, even if a patient was randomized to receive those measures.
The anatomy of a good blog
ICHE recently published an unusual article (which other article has ‘the world wide web’ as their setting) on blogging in ID and clinical micro. The article reviewed around 100 blogs and rated them using a multifaceted tool. The article has some useful qualitative feedback from bloggers and readers, and identifies some gaps in the blogosphere (especially around antimicrobial stewardship). Rachael Troughton, one of the study authors, recently published a post on the article – and here’s my take on it.