Mindful of our need to up our game in terms of communication to non-experts around AMR-related issues, I have been scouting around for a good video to portray the basic of AMR, and came across this by Health Education England. It’s not the best animation that I have seen, but I quite like it – and the strap line at the end is interesting (“Take care. Not antibiotics”). I’d be interested in your views on this video, and please feel free to flag any other good ones out there.
LA-MRSA: On the definition of emergence
Some friends, called patriotic hackers, had secured a very interesting surveillance database and I tried to write a manuscript, when I was scooped (in CID) by friends that apparently had access to the same database. That made my work redundant. So, for your eyes only, my take on that data. Continue reading
WHO IPC Core Components
While I had seen the WHO IPC Core Components, I have totally missed the great video they made. Thus, with no further comment, here the link to this well-made video.
Just in case that the link via the picture doesn’t work, copy and paste the following link into your browser: https://www.youtube.com/watch?v=LZapz2L6J1Q&feature=youtu.be
Friday Afternoon: ATP vs UV vs eyeball Vs K9 and Going Commando in Surgery
 Well I was looking for a Friday afternoon sort of post and you know when you wait a while and two come at once?.. So firstly, some may recall that I have previously highlighted the utility of a sensitive nose in detecting a variety of things in a previous post. In a study just posted online first in the Journal of Hospital Infection, a springer spaniel was trained to detect C. difficile in the environment with a fair degree of success, especially for detecting rooms in which C. difficile was not present. Continue reading
Well I was looking for a Friday afternoon sort of post and you know when you wait a while and two come at once?.. So firstly, some may recall that I have previously highlighted the utility of a sensitive nose in detecting a variety of things in a previous post. In a study just posted online first in the Journal of Hospital Infection, a springer spaniel was trained to detect C. difficile in the environment with a fair degree of success, especially for detecting rooms in which C. difficile was not present. Continue reading
Looking back to see the post-antibiotic era
Now online in Lancet ID an impressive and important retrospective study describing the faith of 437 patients with BSI caused by carbapenamase-producing Enterobacteriaceae (CPE). When scanning the conclusions of your weekly diarrhea of new papers (as I do) this one might have escaped your attention: (in short) “Appropriate therapy is good. Combination therapy too. Patients with BSIs due to CPE should receive active therapy.” Yet, there is much more interesting stuff in this paper. Continue reading
Blog-ception: An article on a blog about an article about blogs
Racheal Troughton (bio below) reports on a fascinating study…As readers of this post are no doubt aware, the community of researchers and clinicians working in infectious diseases are increasingly using social media as a resource, and a platform for scientific discourse. But there is little discussion on precisely how it is being used. Back in 2015, we began a study to analyse the content and culture surrounding blogs in the field of infectious diseases – the “blogosphere”. Continue reading
C. auris questionnaire – the outcome
Overall 61 colleagues from 17 countries answered the questionnaire. A large proportion (26 of 61) of the answers came from the UK, which might have to do with the fact that the first European outbreak was described in England.
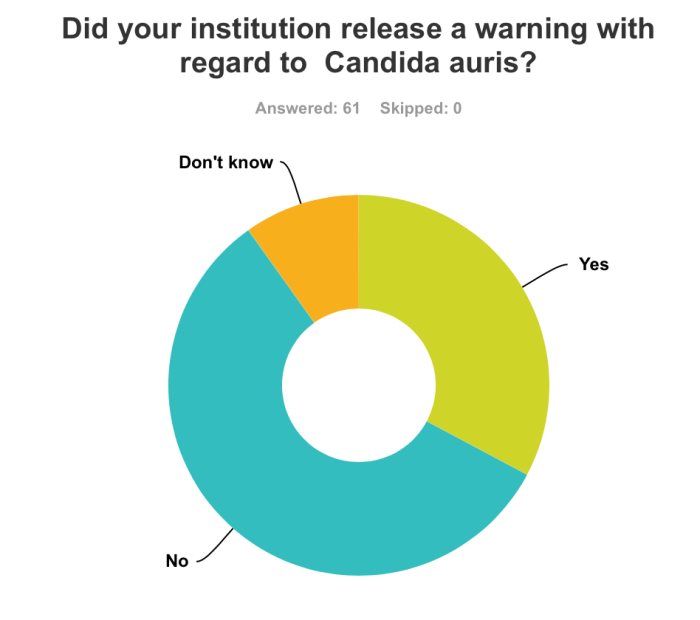
Of the respondents 32.8% said that their institution released a warning about C. auris. Analyzing the data separately for the UK and the other participating countries, it became clear that the first European outbreak had impact on the preparedness. In the UK 42.3% of the institutions were warned about the unique capacities of C. auris, versus 25.7 in all other countries. Regarding the existence of a written guideline dealing with C. auris, the differences were far less pronounced, namely 26.9% versus 20.0%, respectively.
53.9% of the UK responders believe that their lab can correctly diagnose C. auris, versus 31.4% in the other countries. In addition, the proportion of responders, who didn’t know if their lab was prepared, was higher outside the UK (45.7% versus 26.9%, respectively).
Despite the emerging spread of C. auris clusters this questionnaire is an indication that most institutions are not adequately prepared. Obviously the sample is really small, but the outcome was predictable. With an increasing body of literature, including papers on diagnostic methods and infection control measures, we should hope that the situation should change very soon. Thus, don’t lean back, start writing.
Special issue on MDR-GNR
The Journal of Hospital Infection have published a welcome special issue on multidrug-resistant Gram-negative bacteria. The collection includes some updates on epidemiology, staff carriage (again!), clinical microbiology, and patient perspectives on CPE, and is well worth a read.
Candida auris part III. Are you prepared?

MMWR just published on the ongoing transmission of Candida auris in the US, while at the same time PLOS Pathogens came with an excellent review on the topic.
By now I had the debatable pleasure to be around for the birth of a few “superbugs”, but this one is clearly putting a lot of effort into reaching the top of the list. I believe (classical pessimist) that many institutions still ignore this new adversary (or are even unaware), and most certainly have no game-plan to prevent its introduction and consequent spread. In the MMWR publication the current recommendations for C. auris–colonized or infected patients were repeated, with only one change from previous recommendations, namely that a more effective (sporicidal) disinfectant is needed, but I seriously wonder who follows this guidance.
Thus, here it comes, another 30-seconds-questionaire. Why? Because I hope that you will prove me wrong and that we – the infection control people at the frontline – act on threat, instead of re-act once we are overrun.
Link to questions https://www.surveymonkey.com/r/QCK9RWS
References
Notes from the Field: Ongoing Transmission of Candida auris in Health Care Facilities — United States, June 2016–May 2017. Weekly / May 19, 2017 / 66(19);514–515 https://www.cdc.gov/mmwr/volumes/66/wr/mm6619a7.htm?s_cid=mm6619a7_e
Chowdhary A, Sharma C, Meis J. Candida auris: A rapidly emerging cause of hospital-acquired multidrug-resistant fungal infections globally. PLOS Pathogens https://doi.org/10.1371/journal.ppat.1006290 May 18, 2017
Staff screening for MDROs: closing Pandora’s Box
A brave study from the Palmore/Frank group at NIH has opened the Pandora’s Box that is screening staff for MDROs, and, I’m delighted to say, firmly closed it with their findings! Only 3% of staff carried ESBLs, one carried a CPE, and none carried VRE, and this despite extensive contact with MDRO patients for many of the staff sampled!

