Probably the most contentious aspect of the COVID-19 pandemic has been PPE for staff. And within that, the most contentious aspect of PPE has been respiratory protection when caring for patients with confirmed or suspected COVID-19: to FFP or not to FFP? I have been involved in a review of international guidelines to identify variation and track the changes in the guidelines over time. Things have changed as evidence has emerged, but international guidelines still disagree on where and when FFP respirators should be worn when caring for patients with suspected or confirmed COVID-19. The review also tracked variation and changes in recommendations about what should be considered an AGP.
Cast your minds back to January 2020 (if you can remember back that far – I’m not sure that I can!). COVID-19 wasn’t yet called COVID-19, the ‘novel coronavirus’ was classified as a High Consequence Infectious Disease, and we knew very little about transmission routes. This was, looking back, the one and only time the international guidelines were united in terms of respiratory protection, recommending FFP respirators (FFP2/FFP3/N95/N99).
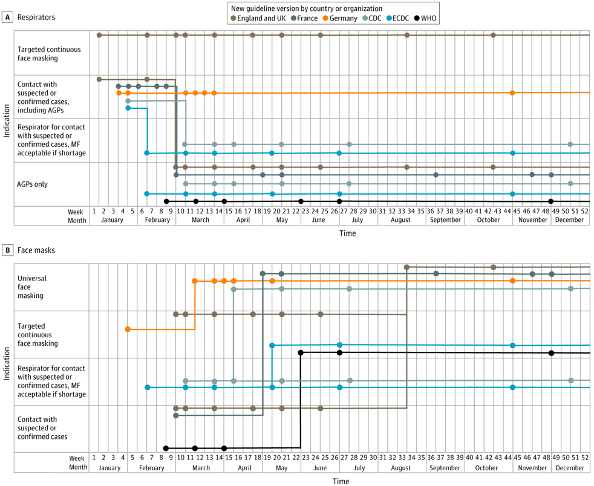
About five or six weeks later, in early March 2020, COVID-19 was declassified as an HCID, and based on emerging evidence, WHO released PPE guidance recommending that surgical masks were sufficient for contact with confirmed or suspected cases and FFP respirators were required only for AGPs. Meanwhile, CDC and ECDC continued to recommend FFP respirators for contact with all suspected and confirmed cases. Countries elsewhere in the world went their own way, in general following with the CDC approach (FFP respirators for contact with all suspected and confirmed cases), or WHO approach (FFP respirators only for AGPs). There were some variations on this theme identified in the review, for example PHE in England recommended FFP respirators in units where AGPs were common (such as ICU, endoscopy, respiratory units etc) in addition to for individual AGPs, and surgical masks for non-AGPs.
There was a parallel evolution in recommendations for when to wear a surgical mask. Guidelines have moved towards universal surgical mask wearing in all healthcare settings (defined as a requirement to wear a surgical mask on entry to a healthcare facility).
The guidelines were not consistent in the designation of an AGP. There was an evolution in the AGP lists in the various guidelines writing groups, with 7 groups providing 13 separate versions of guidelines over the course of the review period. Procedures classified as AGPs varied from 3 to 14 procedures. Intubation and bronchoscopy were the most classified as AGPs, with intubation the one procedure to appear in all 13 guidelines.
As the review concludes, the variation and evolution in international guidelines on respiratory protection and AGP designation has been understandable as evidence has emerged but not very helpful! What is certain is that any PPE carelessly used, especially during doffing, will increase the risk of staff exposure to COVID-19 and other pathogens. So, regardless of your views on which respiratory protection to go for, we can all agree that PPE should be used carefully to reduce the risk of staff contracting COVID-19.
Discover more from Reflections on Infection Prevention and Control
Subscribe to get the latest posts sent to your email.
Jon, this is really interesting. Do you have any idea of the rates amongst German healthcare workers Vs others. I assume there will be too many confounding factors (community Vs occupational acquisition) to do this with any accuracy.
LikeLike
No I don’t but agree would be difficult to draw any hard and fast conclusions due to confounders, as you say. In this review and meta-analysis, HCW in the USA had the highest rate of HCAI, but I don’t think we should read too much into this in the context of FFP vs. surgical mask https://reflectionsipc.com/2021/03/05/how-many-healthcare-workers-have-had-covid-19/
LikeLike