The contrast in the stringency of the CDC and UK Department of Health / Health and Safety Executive guidelines for infection prevention and control when dealing Ebola virus disease (EVD) patients is striking. This is particularly acute with regard to recommendations for Personal Protective Equipment (PPE) and terminal disinfection. Having recently reviewed both documents for a webinar on Ebola infection prevention and control (you can download the slides here, by the way), I thought I’d share the contrast:
Table: PPE and disinfection recommendations for dealing with patients with Ebola virus disease. Source: US CDC patient and environmental guidelines, and UK Department of Health. (Please note – this summary chart is designed to be illustrative rather than definitive.)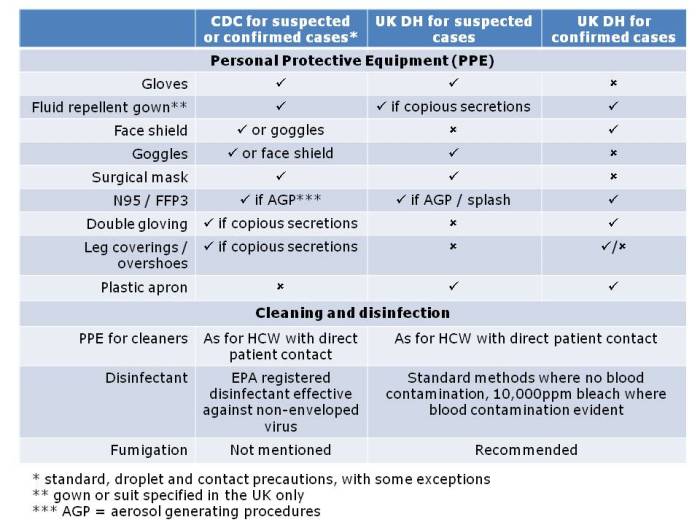
So is there any reason why the level of PPE and type of terminal disinfection required should be any different depending on which side of the Atlantic you happen to be? None whatsoever. So why the discrepancy? It’s difficult to say. This difference in recommendations has prompted the question of “To CDC or not to CDC” in terms of PPE for Ebola, and an opinion piece in Annals of Internal Medicine justifying the CDC approach. It is probably true that the level of PPE recommended by CDC is enough to block transmission, and that the risk of environmental contamination is low enough such that fumigation is not necessary. Probably. But is that good enough when Ebola is on the line? It is certainly true that you can be wearing all the PPE in the world but if you put in on incorrectly, don’t take care of it during use or remove it carelessly you will put yourself at risk.
When I came to decontaminate a room using hydrogen peroxide vapour following a case of Lassa fever in London some years ago, I wore all the PPE that I could lay my hands on (see below)!
Me illustrating the “belt and braces” (aka paranoid) approach to PPE (a la UK, not CDC recommendations).
Did this level of PPE match the risk of exposure to viable Ebola? Perhaps not, but it certainly made me feel a whole lot more secure about entering the room to do the job!
Discover more from Reflections on Infection Prevention and Control
Subscribe to get the latest posts sent to your email.
Thanks Jon for this informative and critical look at the discrepancies in handling dangerous pathogens. As we all know, the environment (here, AKA terminal room fumigation or deep cleaning) has become an important piece in the puzzle to fighting not only Ebola and other headline agents, but just as important for HAIs and other easily transmissible agents after a patient has vacated their room (“environment”).
LikeLike
Thanks Rodney – I’m sure that the environmental reservoir is much more important for many regularly healthcare-associated pathogens (C. difficile, VRE, Acinetobacter baumannii and norovirus) than for Ebola. But the consequence of acquisition is so great that I do think enhanced procedures aimed at all possible transmission routes are justified for Ebola.
LikeLike
Why is there an x in gloves, goggles and surgical mask under the column UK DH for confirmed cases? I understand the x by the surgial mask since you have checked N95 but why no goggles or gloves with confirmed cases?
LikeLike
Thanks for the comment Laurie. I have unchecked gloves, but checked double gloves; unchecked surgical mask, but checked N95 (FFP3); and UK guidelines recommend face shield (rather than ‘eye protection’, which is specified for high-risk unconfirmed cases) for confirmed cases. The terminology used in the US and UK guidelines is different, so it wasn’t easy to produce the direct comparison chart – which should be seen as illustrative rather than definitive.
LikeLike
Jon, here in the U.S. we call such precautionary steps the equivalent of wearing a belt and suspenders; better be safe than sorry. I agree with you that the best PPE is worthless if worn inappropriately. Having been in the cleaning and disinfection business in hospitals for the past 33 years, I advocate using ultra microfiber cloths to clean, then disinfect (2 step process) environmental surfaces while wearing whatever makes the cleaning person feel safe and secure. I like your photo of what you wore when cleaning the room with Lassa Fever. Keep up the good work!
LikeLike
Jon,
There will always be paranoia present in both professionals and laymen. It’s human nature to fear what is unknown and pull back to what one knows or believes is known.
Perhaps the most likely path of and opportunity for exposure will be when the “relief” of finishing the tasks that present exposure gives way to complacency while removing all levels of PPE. Religiously adhering to proven processes should be as important to HCWs as PPE.
LikeLike
Hello Jon,
What would be your recommended protocol for decontamination of worn PPE after exposure to Ebola?
My understanding is that currently in Africa, health workers essentially mist bleach over their PPE. Do you know if the PPE is then reusable, or disposed of?
And in terms of disinfecting vehicle interior surfaces after patient transport, is the vehicle misted with bleach and left to evaporate? Or is the bleach wiped off?
-Coming from a student who is very interested in learning more about infectious diseases and microbiology!
LikeLike
Hi there, thanks for these excellent questions. I’m afraid I can’t answer the one about decontamination of PPE in field settings. I suggest you contact WHO / MSF about this. I’m only familiar with hospital protocols, where single use disposable PPE is specified.
In terms of emergency vehicles, some hospitals have used hydrogen peroxide vapor to decontaminate ambulances. It’s not a good idea to ‘fog’ bleach or most other chemicals due to health and safety concerns. Meanwhile, other hospitals & healthcare services take the view that emergency vehicles can be disinfected manually using bleach or some other liquid disinfectant.
LikeLike
If you follow the CDC guidelines for PPE in a confirmed Ebola case with simple mask….you’re nuts!! This is not good enough! If level 4 containment suits are good enough for CDC lab personnel, its good enough for nurses caring for patients with Ebola!!!
LikeLike
Note, CDC have since ‘upgraded’ their PPE recommendations to be more in line with UK guidance: http://www.usatoday.com/story/news/nation/2014/10/20/cdc-new-protocol/17638161/
LikeLike
Do personal protective equipment have a coating which changes color when in contact with bodily fluids? This benefits practice sessions and actual conditions. Knowing the location of fluids alerts one prior to doffing. Too much contact may mean increased susceptibility to exposure to skin. Something about good, better, and best!
LikeLike
That’s a really good idea. Current PPE does not do this – but somebody should look at it! There was a recent opinion piece in JAMA seeking better PPE for Ebola: http://jama.jamanetwork.com/article.aspx?articleid=1920943
LikeLike
Thank-you. The coating could be administered by a quick drying aerosol spray. Written to (TNTC) too numerous to count sources and will continue until . . . !
LikeLike
Could a redesigned cooling towel help comfortability and prolong focus?
LikeLike
Maybe, but you may need to explain what one is first!
LikeLike
Check out http://www.chillskinz.com.
LikeLike
Check out via google or bing “chillskinz video” lasting 1:45.
LikeLike
Dear Jon: After weeks of thinking I finally reached the end of my expertise.
Do personal protective equipment have a coating which changes color when in contact with bodily fluids? A litmus solution made of cabbage with a quick drying agent delivered by an aerosol spray is applied to the personal protective equipment. All bodily fluids have a ph.
Knowing the location of fluids alerts one prior to doffing. Too much contamination increases the susceptibility of exposure.
A redesigned cooling towel can prolong comfort and focus.
Glenwrick Elliott, RN
ps Thank-you!
LikeLike
Do You know anything about NHS England Innovation Exchange? Ref: http://www.england.nhs.uk
LikeLike