A recent US study has investigated CPE contamination of sinks, drains, and wastewater. Carbapenemase-producing bacteria were identified throughout the drainage and water system, from drains in patient rooms, right through to wastewater sampled through manholes adjacent to the hospital. My main question in all of this is whether this huge reservoir of carbapenemases in hospital wastewater is a risk for patients. The lack of genetic similarity between isolates in hospital wastewater and isolates from patients suggest not, but I suspect there’s an indirect link and these carbapenemases find their way into isolates affecting humans, which is supported by genetic links between the plasmids carrying the carbapenemases.
There is emerging evidence that the wet and dry contaminated environment can be a risk for CPE transmission. Sinks are often contaminated (although cause and effect is difficult to establish). And beyond sinks, hospital sewage and wastewater are known reservoirs of carbapenemase-producing organisms.
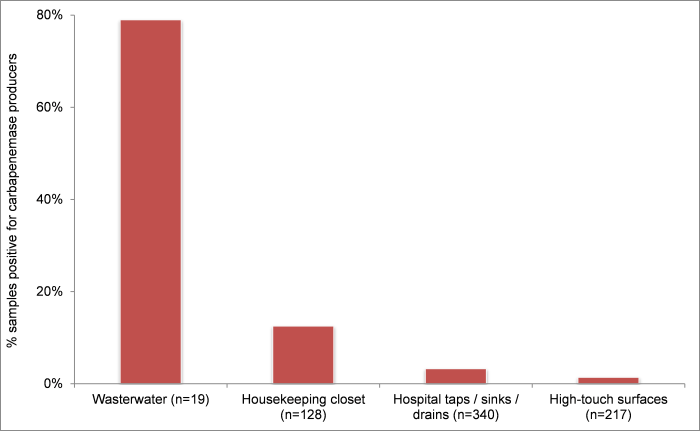
In this context, the National Institutes of Health Clinical Centre (a unique research hospital in the US) report the findings of an extensive environmental screening programme, covering high-touch surfaces in the clinical environment, sinks and drains in the hospital, and wastewater coming out of it. A real surprise was the massive rate of contamination of hospital waste water with carbapenemase-producing organisms – 80% of samples (Figure 1). All seven wastewater samples collected from the intensive care unit (ICU) water pipe system contained at least one carbapenemase-producing organisms, whereas wastewater samples from other wards contained no carbapenemase-producing organisms. This suggests an unexpected and huge reservoir in the pipework in the hospital water supply and beyond. In contrast, the rate of contamination on high-touch surfaces in the hospital itself was low – just 1% of 217 surfaces.
Figure 1: Rate of contamination of environmental samples with carbapenemase-producing organisms.
The study used WGS to link patient and environmental isolates. 8 of 36 carbapenemase-producing organisms from patients were linked to environmental isolates – but all of these were from samples taken in the hospital either from high-touch surfaces, or sinks and drains in clinical or cleaning areas. None of the patient isolates were linked to wastewater samples. Related to this, the rate of AMR was higher in the patient isolates then in the environmental isolates. So, it seems that the huge resevoir of carbapenemases in wastewater were not directly related to carbapenemases in patients, but it seems likley that carbapenemase-encoded plasmids in hospital wastewater do find their way into patient populations due to genetic similarity in the plasmids themselves. We know that wastewater treatment does not get rid of carbapenemases, so humans outside of hospitals come into contact with carbapenemase-encoded plasmids with their origin in waste water, which find their way into bacteria adapted for human colonisation / infection, and humans outside of hospitals find their way into hospitals (as patients, visitors…and staff). So, there’s a very plasuible (if rather circuitous) route for carbapenemases in wastewater to end up in clinical isolates.
This comprehensive study certainly moves the discussion on the role of inanimate reservoir for carbapenemase-producing organisms forwards, suggesting that hospital wastewater could be a major and under-discussed risk.
Discover more from Reflections on Infection Prevention and Control
Subscribe to get the latest posts sent to your email.
Hi Jon, thanks for this. We had two outbreaks of MDR Pseudomonas aeruginosa and theorised that our outbreak strain was, and still likely is, in the waste pipes as cases occurred when there was an efflux of waste water back up the drains into the clinical areas.
LikeLike