BMC Medicine have recently published a study from researchers in Oxford, PHE, and Manchester illuminating the importance of referral networks in the transmission of CPE. The bottom line is that regional referral networks seem to be the most important driver of CPE spread, such that a small CPE problem close to home is more of a threat than a larger CPE problem in a distant referral network!
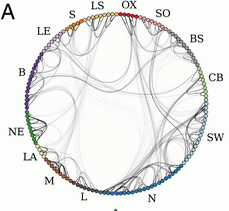
The authors cleverly (and actually rather beautifully) used NHS-HES data to redraw the map of England based on patient referral networks (Figure 1). Interesting to note that the connections between referral networks seem to map pretty closely to motorway road network. (Yes, I am a man in my late 30s who likes nothing more than motorway chat. And boiler chat.) Note the M40 between North London (N) and Oxford (OX), the M3 between Hampshire (S) and South London (SW), and the M5 between the South West (BS) and Birmingham (B)!
Figure 1. The English patient referral wheel. (I work in the tangled spaghetti that is London North (‘N’ on the wheel))!
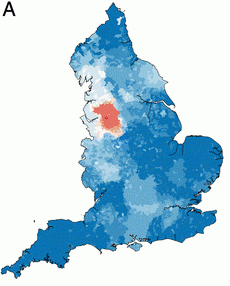
The team then overlaid CPE data from the voluntary PHE national collection onto the referral network. This identified, as you would expect, a KPC hotspot in the Manchester region (Figure 2).
Figure 2: KPC hotspot in the Manchester referral network.
It seems that most CPE introductions come from hospitals within a regional referral network, even if the prevalence in another referral network is much higher (more than 100x higher, in fact)! Who to screen? There’s a helpful, simple example in the discussion to help us get our heads around this concept: ‘If 50% of two patients received from a high-risk hospital are colonised, this one patient poses a lower onward transmission risk if unidentified than 1% colonised patients out of 1000 patients previously admitted to the same hospital (10 patients).’ The researchers modelled what would happen if (when!) CPE prevalence increased, and perhaps surprisingly, the importance of hospitals outside of a regional referral network decreased!
These findings have some important implications for how we approach CPE screening. Current PHE guidelines recommend screening patients from “high-risk” hospitals. However, these findings suggest that we should focus more on admissions from our own region. Whilst prevalence may well be lower, the absolute risk of introducing CPE will be higher. Unfortunately, this means a larger volume of CPE screening. But well worth the investment in my view, given the mammoth cost of CPE outbreaks!
The main limitation of the study is that it is skewed by the national voluntary dataset used, which I think is at least a 10-fold underestimate of the true prevalence of CPE. The authors do acknowledge this important limitation, but worth underlining.
There is a temptation to “Trust nobody – especially not your neighbours” and slide into ‘sibling rivalry’ (look at the fierce football related rivalry between Southampton and Portsmouth, Manchester and Liverpool, or Arsenal and Tottenham)! But if we are to be effective in containing the spread of CPE, we need to work regionally, and this study outlines a pretty good starting point in defining healthcare regions in England!
Discover more from Reflections on Infection Prevention and Control
Subscribe to get the latest posts sent to your email.