There’s surprisingly little literature published on the cost of HCAI outbreaks. In this context, a useful Dutch study in PLoS ONE counts the cost of 7 HCAI outbreaks.
outbreaks
Look out: resistance outbreaks about!
We are all familiar with the idea of outbreaks. A noteworthy pathogen rears its ugly head leaving a trail of destruction in its wake (as in ‘Contagion’, or before that, ‘Outbreak’). (I credit ‘Outbreak’ with getting me into microbiology and epidemiology as an impressionable 15 year old by the way.) Or more commonly in hospitals, a ward experiences an increased incidence of a particularly resistant or virulent clone. But a recent study from some colleagues at the Centre for Clinical Infection and Diagnostics Research at St. Thomas’ Hospital in London turns the idea of ‘outbreak’ on its head by identifying surprisingly common outbreaks of resistance to a particular antibiotic across different species.
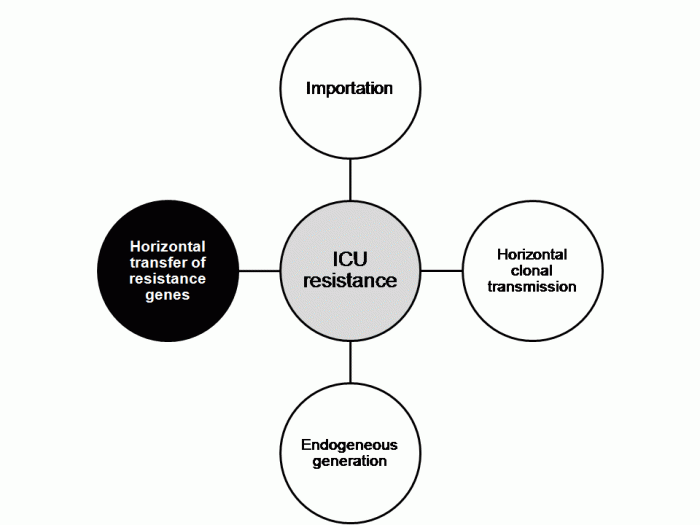
The horizontal transfer of resistance genes is generally considered to be a rare event relative to horizontal, clonal transmission of an outbreak pathogen (see Figure below). But the findings of this study suggest more promiscuous spread of resistance genes than you may expect.
Figure: Horizontal transfer of resistance genes is generally considered to be the least common cause of ICU resistance.
The team used some outbreak scanning software to interrogate laboratory reports from two ICUs between 2002 and 2009. Analysis of the large dataset, comprising almost 90,000 patient days, found that outbreaks occurred for two thirds of the 26 ‘species-groups’ studied. Only three of these were recognized at the time. Thirty-nine outbreaks of resistance were detected, the majority of which (87%) did not coincide with an increase in a particular ‘species-group’, supporting the fact that these were due to horizontal gene transfer between species.
The clustering of individual species into ‘species-groups’ is somewhat problematic, and may serve to over-emphasize the number of outbreaks that occurred. Quite a number of the outbreaks of the same ‘species-group’ and of resistance were very small – with 2 cases over a day or two. Also, clustering of the same species does not necessarily mean clonal transmission has occurred – you’d need to do molecular typing to prove that. Similarly, clustering of resistance across species to the same antibiotic does not necessarily mean horizontal gene transfer has occurred; multiple mechanisms could be involved. Notwithstanding these limitations, this is an important study and has changed the way that I think about hospital outbreaks.
Infection control interventions implemented to control recognized outbreaks on the ICU appeared to reduce the overall number of outbreaks of the same ‘species-group’, but did not affect the number of resistance outbreaks. So, it seems that different measures are necessary to control outbreaks of resistance. Perhaps the best weapon we have to combat outbreaks of resistance is to restrict our use of antibiotics. If we can reduce the selective pressure driving resistance, we should see less clonal outbreaks of resistant bacteria and less resistance outbreaks across species.