The 2018 ESPAUR report was published a few weeks ago. It’s freely available for your perusal here, and packed full of juicy info. Here’s a few reflections on the report.
- CPE referred to the reference lab have not topped 3k. As I’ve said previously, this is a gross underestimate of CPE prevalence in England. The amount of CPE out there is at least 10x this figure, and probably more than 100x.
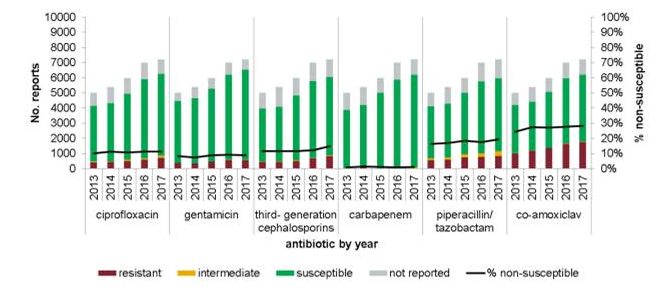
- >98% of Kleb and E. coli BSIs remain phenotypically susceptible to carbapenems, so England remains firmly in the ‘green’ in terms of ECDC heatmaps – but no room for complacency. Not least because the actual number of antibiotic resistant Gram-negative bacteria is increasing notably in proportion to the increase in all GNBSI (see Figure 1 below).
- Total antibiotic use increased by 6% between 2010 and 2013, but has now reduced by 6% between 2014 and 2017.
- The main bulk of antibiotic prescribing is in primary care (81%), and there were 13% fewer antibiotic prescriptions dispensed comparing 2017 with 2013.
- However, in hospitals, antibiotic use continues to rise by 2% (see Figure 2). This represents a slowed rate of increase – antibiotic use in hospitals rose by 12% between 2010 and 2013. But should we be celebrating a reduction in the rate of increase in the use of antibiotics in hospital?? Perhaps – but let’s reserve the full-blown party for when antibiotic use actually declines in hospitals!
- Related to this, slightly depressingly, only 23% of Trust managed to meet their CQUIN target for reducing total antibiotic consumption, and only 45% managed to meet their CQUIN target for carbapenem consumption. Amazingly, 25% of Trusts managed to fail to meet the CQUIN target for reducing piperacillin/tazobactam consumption, despite the fact that there was almost none of it available. Not sure how they managed that.
- There’s a section summarising the largely successful interventions to control the spread of Candida auris in England hospitals.
- Some interesting modelling work suggests that 17% of antibiotic therapy days in secondary care are unnecessary.
- The TARGET antibiotic tools and resources are proving popular and useful.
- The report includes and evaluation of the Keep Antibiotics Working, Antibiotic Guardian, and e-bug
We’re lucky to have this report – thanks to all who have put it together.
Figure 1: The increasing threat from antibiotic resistant Klebsiella pneumoniae
Figure 2: Antibiotic consumption in NHS acute hospitals
Discover more from Reflections on Infection Prevention and Control
Subscribe to get the latest posts sent to your email.